Brief Case Description
The patient is a 60 year-old female with a recent history of non-ST-elevation anterior myocardial infarction and congestive heart failure. She has a past medical history of hypertension, diabetes, hyperlipidemia, peripheral vascular disease, stroke and remote myocardial infarction. She has a known history of coronary artery disease with multiple previous percutaneous coronary interventions.
Transthoracic echocardiography (TTE) showed type IIIb mitral valve dysfunction with predominantly restricted leaflet motion of the posterior leaflet (parasternal long axis and four chamber views). Doppler echocardiography showed moderate mitral regurgitation with a posteriorly directed jet. Quantitative measurement revealed a regurgitant orifice area of 28 mm2 and a regurgitant volume of 46 mL. Pisa radius was calculated at 0.8 cm. Left ventricular end diastolic diameter was 5 cm and left ventricular ejection fraction was 33%.
Cardiac catheterization showed severe three vessel coronary artery disease: left anterior descending artery with mid total occlusion, first obtuse marginal 80% in-stent restenosis, proximal right coronary artery 70% in-stent restenosis, and posterior descending artery (PDA) branch 95% stenosis. Left ventricular ejection fraction was 30%.
The patient was referred for coronary revascularization and reconstructive mitral valve surgery.
Operative Procedure
Intraoperative Transesophageal Echocardiography (TEE)
Intraoperative transesophageal echocardiography confirmed the diagnosis of type IIIb mitral valve dysfunction (mid esophageal long axis and four chamber views). Doppler echocardiography showed mild (2+) mitral regurgitation with a central jet (mid esophageal four chamber and mitral commissural views). A transgastric basal short axis view of the mitral valve is also shown.
In this case, we observed a reduction in the severity of mitral regurgitation when comparing preoperative TTE with intraoperative TEE. It is important to note that intraoperative TEE often downgrades the severity of mitral regurgitation in patients with type IIIb dysfunction. The mechanism underlying this phenomenon is the unloading effect of general anesthesia which results in arterial and venous dilatation, decreasing afterload and preload respectively.
Coronary Artery Bypass Grafting (CABG)
The patient underwent coronary artery bypass grafting with the left internal mammary artery to the left anterior descending artery and saphenous vein graft from the aorta to the obtuse marginal and PDA branches.
Mitral Valve Analysis
Following the exposure of the mitral valve, we first confirmed the echocardiographic findings by observing a tethering of both anterior and posterior leaflets which predominated at the level of P2, P3, and PC area. There was also a significant deformity of the posterior mitral annulus.
Following this echocardiographic and operative valve analysis, we can summarize the pathophysiological triad as follows:
Etiology: Ischemic mitral valve disease
Lesions: papillary muscle displacement with leaflets tethering, and secondary annular deformity
Dysfunction: Type IIIb
Reconstructive Procedure
The patient underwent an undersized remodeling mitral annuloplasty with the implantation of a size 28 mm Carpentier-McCarthy-Adams IMR ring.
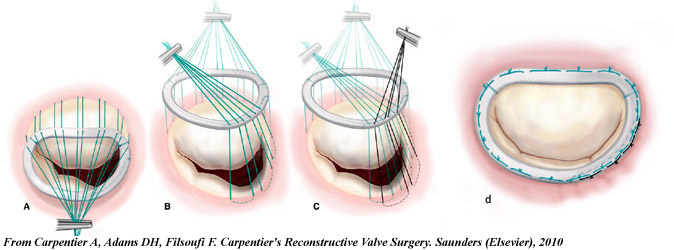
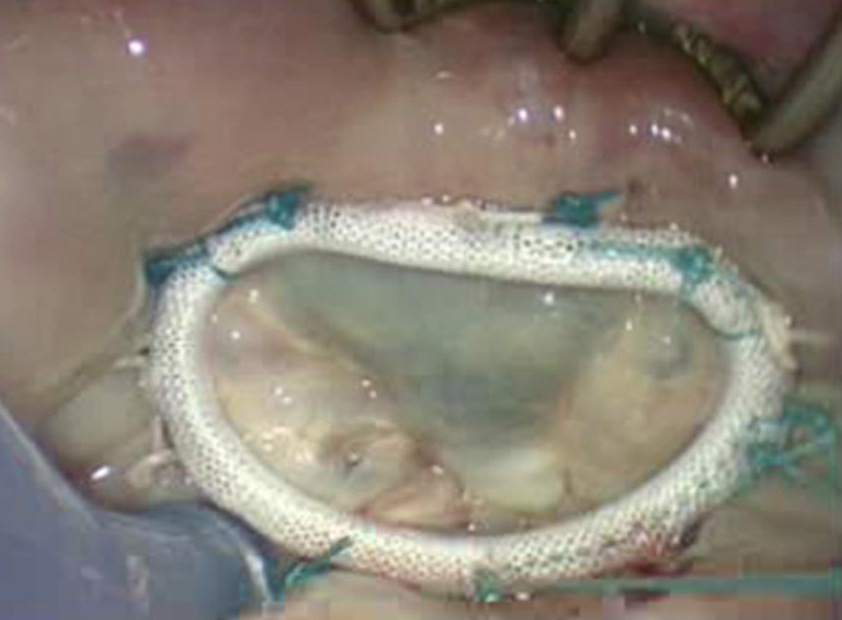
Postbypass Transesophageal Echocardiography
Postbypass transesophageal echocardiography showed a competent mitral valve with minimal residual regurgitation.
Transgastric basal short axis, mid esophageal mitral commissural and four chamber views showed the mitral valve with good leaflet coaptation. Mid esophageal long axis view with color Doppler interrogation showed a competent mitral valve with no residual regurgitation.
The postoperative course was uneventful and the patient was discharged home on postoperative day seven.