Brief Case Description
The patient was a 31 year-old female with a past medical history of rheumatic fever who presented with symptoms of congestive heart failure. She had been diagnosed with mitral stenosis and underwent percutaneous mitral balloon dilatation a few years earlier.
Transthoracic Echocardiography (TTE)
Transthoracic echocardiography showed type IIIa mitral dysfunction (restricted leaflet motion in diastole and systole) with the thickening of both mitral valve leaflets. There was a moderate diastolic doming of the mitral valve. The posterior leaflet appeared retracted and the subvalvular apparatus was thickened with visible chordae. On Doppler echocardiography there was a posteriorly directed jet with significant mitral regurgitation. Mitral valve area was calculated at 1.7 cm2. The effective regurgitant orifice area was 39 mm2. The regurgitant volume was 70 mL. There was also Type I dysfunction of the tricuspid valve with mild to moderate regurgitation. Left and right ventricular functions were preserved.
In the presence of symptomatic severe mitral regurgitation and moderate tricuspid regurgitation, the patient was referred for reconstructive valve surgery.
Intraoperative Transesophageal Echocardiography (TEE)
Intraoperative TEE (mid esophageal four-chamber view) confirmed the diagnosis of type IIIa mitral valve dysfunction with the thickening of both leaflets and the retraction of the posterior leaflet. On Doppler echocardiography, the jet of mitral regurgitation was more central in four-chamber view. Three dimensional echocardiography showed that posterior leaflet shortening was predominant at the level of P2 and P3 segments. The mobility of the anterior leaflet was preserved on 2D and 3D echocardiography which is an important consideration for reconstructive valve surgery.
Mitral Valve Analysis
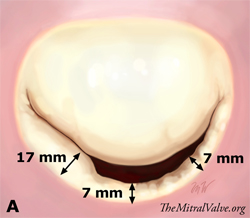
Intraoperative valve analysis confirmed the findings of echocardiography by demonstrating type IIIa dysfunction. As expected, mitral valve lesions were multiple and complex and could be summarized as follows:
Reconstructive Procedure
Valve reconstruction was considered feasible in this particular case as the pliability of the anterior leaflet was preserved and the subvalvular lesions were not severe and extensive.
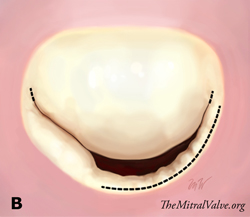
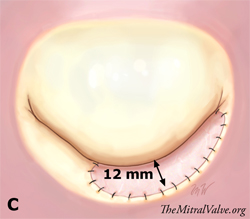
First, an anterolateral and posteromedial commissurotomy was performed. Then, the posterior leaflet was transversally incised at P2 and P3 segments a few millimeters from the annulus (Fig B). The adequate exposure of the ventricular aspect of the leaflet enabled us to resect all secondary chordae attached to P2 and P3 segments to increase its mobility. An oval-shaped glutaraldehyde preserved autologous pericardial patch was tailored and used for extension of the posterior leaflet. The maximum height of the patch was 12 mm and its length was equal to the length of P2-P3 segments (Fig C).
The 12 mm height was calculated in order to obtain a similar final shape and height between P2, P3 and P1 segments and considering that 2 mm of the patch was used circumferentially for suturing.
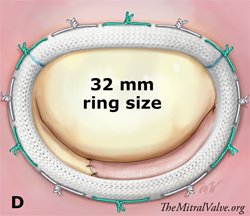
Finally, a prosthetic ring annuloplasty was performed. Ring selection is based on the measurement of the anterior leaflet. In this case, a 30 mm sizer was covering the surface area of the anterior leaflet. The selected ring, however, should take into consideration the surface area of the reconstructed posterior leaflet. The use of patch extension enabled us to implant a 32 mm ring (one size greater than the sizer covering the anterior leaflet surface area) (Fig D).




Furthermore, the patient underwent a tricuspid ring annuloplasty.
Postbypass TEE showed a competent mitral valve with minimal transvalvular gradient. The posterior leaflet pericardial patch extension was well visualized on TEE. The postoperative course was uneventful.
For more information refer to Current Status >> Rheumatic Valve Disease Section